Also known as a “spinal tap,” a lumbar puncture is used to diagnose life-threatening diseases, administer medications, and measure intracranial pressure. An estimated 360,000 of these procedures are performed annually in the U.S. for various purposes.
However, that doesn’t mean they’re simple bedside procedures.
As the lumbar fat increases, it becomes more difficult to perform. Landmarks also become harder to palpate with increasing subcutaneous fat. This is why it’s important to thoroughly understand the latest studies. They suggest that ultrasound guidance for lumbar puncture (LP) could improve success rates, decrease needle redirections and traumatic taps, and decrease total procedure time.
The correct technique and necessary precautions can further minimize risks. Learn all about it when you register for our comprehensive Lumbar Puncture course.
Step 1: Assessment
Is your patient a good candidate for lumbar puncture? A proper assessment will help you decide.
Indications
A lumbar puncture can be indicated for diagnostic and therapeutic purposes in cases of:
- CNS syphilis
- Altered mental status (AMS)
- Leptomeningeal CNS lymphoma
- Suspected subarachnoid hemorrhage
- Suspected meningitis or encephalitis
- Nuchal rigidity, which is a symptom of bacterial meningitis. Prompt LP could decrease mortality and increase favorable outcomes with no hearing deficits.
- Suspected meningeal carcinomatosis, cryptococcal, and tuberculous
- Inflammatory and neurological conditions like Guillain-Barre syndrome, multiple sclerosis, and transverse myelitis.
It can also be used for therapeutic purposes, such as intrathecal injection of antibiotics, baclofen, and chemotherapeutic agents, spinal anesthesia, therapeutic drainage of CSF, or when injecting contrast media for a CT myelogram or cisternography.
Contraindications
There are some conditions where LP can do more harm than good. We’ve outlined them here, so you know where it’s contraindicated and when you need to mitigate risks. That said, you should always weigh the risks against the potential benefits, as a lumbar puncture may be necessary in some cases despite contraindications.
- Skin infection near or at the insertion site
- International normalized ratio (INR) > 1.5
- Central nervous system (CNS) lesion or spinal mass
- Platelet count of < 50 × 10(9) /l or thrombocytopenia
- Use of anticoagulants in the past 24 hours. Research shows they can increase the risk of hemorrhagic complications.
This also includes elevated intracranial hypertension (pseudotumor cerebri) due to increased CSF pressure, obstructive hydrocephalus, or Arnold-Chiari malformation.
Risk factors include AMS (LR 2.2), focal deficit (LR 4.3), and Papilledema (LR 11).
In this scenario, a CT is typically ordered before performing a lumbar puncture to avoid the risk of brain herniation. However, should midline structures experience a lateral shift, basilar and suprachiasmatic cisterns are lost, the fourth ventricle is obliterated, or the quadrigeminal and superior cerebellar plate cisterns with sparing of the ambient cisterns are obliterated, these must be regarded as contraindications.
Step 2: Understanding Complications
A lumbar puncture is regarded as a generally safe procedure, with side effects like headache, bleeding, back pain, and swelling that typically go away after a few days.
Major complications from a lumbar puncture are rare, but can include:
- Lower limb paresthesias, affecting 0.3% of patients
- Cerebral herniation, occurs in 5% of patients with acute bacterial meningitis (ABM)
- Epidural abscesses, experienced in 0.2 to 2.8 cases out of every 10,000 per year
- Postdural puncture headache, which varies between 10% to 40%
- Spinal hematoma happens among 0.20% of patients without coagulopathy and 0.23% for those with coagulopathy
There’s also a risk of diskitis, an uncommon but incredibly serious complication.
Step 3: Gathering Equipment
The ideal lumbar puncture kit varies across patient characteristics and concerns, but there are some items that are fundamentally necessary for safe and effective procedures.
These include:
- Sterile gloves
- cap
- Disinfecting betadine solution
- Syringes with needles
- Sterile drapes
- Local anesthetic (1% lidocaine)
- Sterile vials for CSF collection
- Spinal manometer with a 3-way valve
- Spinal needle with a stylet
Whenever possible, opt for a pencil-point 25G Whitacre spinal needle instead of a Quincke needle. The former has lower risks of post-dural puncture headache (PDPH).
Step 4: Getting Started on the Procedure
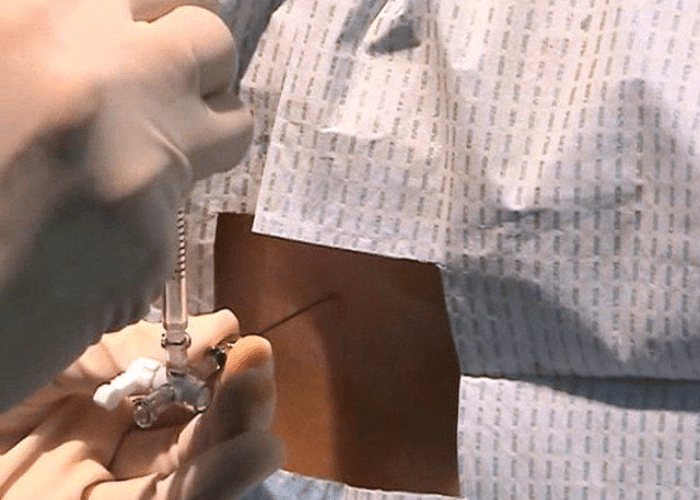
- Ask the patient to sit or lie in a lateral recumbent position, with the hips and shoulders in the same plane. The latter is preferred as it allows an accurate measurement of opening pressure.
- Have them curl into a fetal position to achieve maximum flexion of the spine. This position increases the interspinous distance, making it easier to insert the needle.
- Position the needle at the midline, going for the L3-L4 or L4-L5 interspace to avoid damaging the conus medullaris—the terminal end of the spinal cord.
- Palpate the skin and mark the area with a skin marking pen for visualization.
- Adopt the aseptic technique, prepping the back with a disinfecting agent. Apply the disinfectant in widening concentric circular movements, starting from the insertion site. Allow the skin to dry and cover it with sterile drapes.
- Apply a local anesthetic, identify the landmarks, and insert the spinal needle at the injection site at an angle of approximately 15 degrees.
- Do this with the stylet in place, holding the needle in the sagittal plane to avoid injury to the dura mater and reduce the risk of CSF leakage after LP.
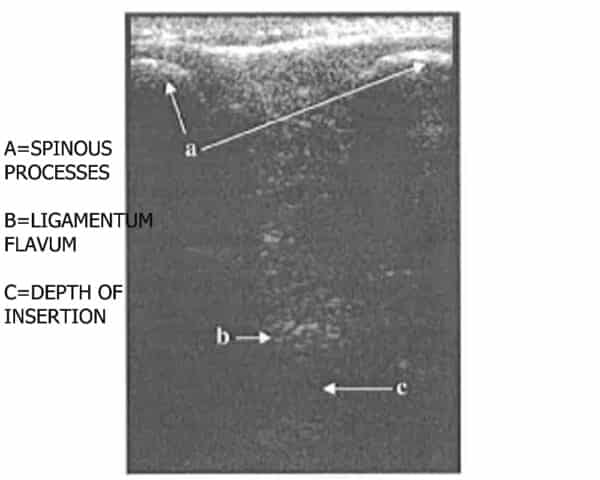
- Advance the needle until a “pop” is felt. This is an indication that you’ve passed through the ligamentum flavum. Slowly and carefully advance the needle in 2 to 3-millimeter increments, removing the stylet each time to check for CSF fluid.
- Attach the manometer to the needle with the stopcock to read the opening pressure.
- Collect 2 milliliter samples in each of the 4 tubes. Replace the stylet before removing the needle. This will reduce the incidence of post-lumbar puncture syndrome. Look for blood or xanthochromia in the CSF fluid as it can indicate that the patient is suffering from an acute subarachnoid hemorrhage (SAH).
- Cover the insertion point with a sterile bandage.
While the procedure is pretty straightforward, locating anatomical landmarks can be difficult. Research has found that ultrasound of the spine in adults can guide lumbar punctures and be helpful. It is successful in 90% of patients compared to landmark-based LP’s 81.4%.
These benefits have been backed by a 2020 article on overweight patients. It showed that the group who underwent ultrasound-guided LPs had a higher success rate of 92.7% compared to 68% among those who underwent LPs without ultrasound guidance. The time to perform was also faster—17.02 minutes vs 37.63 minutes. Clearly, the ultrasound of spine in adults requires fewer needle insertions and redirections.
Conclusion
Ultrasound of spine in adults plays an important role in lumbar punctures. Unfortunately, not many healthcare providers are not well-versed in administering it. Hospital Procedures Consultants is committed to changing that through programs like the Spine Ultrasound Course. With additional training, your patients can benefit from ultrasound-guided lumbar punctures’ higher success rate as you enrich your clinical skills.
Resources:
Short, A. Dunneback, E. Stephens, J. Guidici, J. Chatterjee, A. Finn, E. Contarino, M. Spangler, H. Heath, J. McEntee, J. Donohoe, A. Hemsey, D. Moore, C. Sturkie, E. Kumfer, A. Campbell, R. Dancel, R. Safety and predictors of the success of lumbar punctures performed by a medicine procedure service. J Hosp Med. 2023 Aug;18(8):661-669. doi: 10.1002
Hudgins, P.A. Fountain, A.J. Chapman, P.R. Shah, L.M. Difficult Lumbar Puncture: Pitfalls and Tips from the Trenches. AJNR Am J Neuroradiol. 2017 Jul; 38(7): 1276–1283
Soni, N.J. Franco-Sadud, R. Schnobrich, D. Dancel, R. Tierney, D.M. Salame, G. Restrepo, M.I. McHardy, P. Ultrasound guidance for lumbar puncture. Neurol Clin Pract. 2016 Aug; 6(4): 358–368. doi: 10.1212
Gottlieb, M. Holladay, D. Peksa, G. Ultrasound-assisted Lumbar Punctures: A Systematic Review and Meta-Analysis. Meta-Analysis Acad Emerg Med. 2019 Jan;26(1):85-96. doi: 10.1111
Glimåker, M. Sjölin, J. Åkesson, S. Naucler, P. Lumbar Puncture Performed Promptly or After Neuroimaging in Acute Bacterial Meningitis in Adults: A Prospective National Cohort Study Evaluating Different Guidelines. Clin Infect Dis . 2018 Jan 18;66(3):321-328. doi: 10.1093
Ning, S. Kerbel, B. Callum, J. Lin, Y. Safety of lumbar punctures in patients with thrombocytopenia. Vox Sang. 2016 May;110(4):393-400. doi: 10.1111
Domingues, R. Bruniera, G. Brunale, F. Mangueira, C. Senne, C. Lumbar puncture in patients using anticoagulants and antiplatelet agents. Arq Neuropsiquiatr . 2016 Aug;74(8):679-86. doi: 10.1590
Salazar, L. Hasbun, R. Cranial Imaging Before Lumbar Puncture in Adults With Community-Acquired Meningitis: Clinical Utility and Adherence to the Infectious Diseases Society of America Guidelines. Clin Infect Dis. 2017 Jun 15; 64(12): 1657–1662. Gower, D. J. Baker, A. L. Bell, W. O. Ball, M. R. Contraindications to lumbar puncture as defined by computed cranial tomography. J Neurol Neurosurg Psychiatry. 1987 Aug;50(8):1071-4.
Joffe, A. R. Lumbar puncture and brain herniation in acute bacterial meningitis: a review. J Intensive Care Med. 2007 Jul-Aug;22(4):194-207. doi: 10.1177
Chao, D. Nanda, A. Spinal epidural abscess: a diagnostic challenge. Am Fam Physician. 2002 Apr 1;65(7):1341-6.
Weji, B. Girma. Obsa, M. Suleiman. Melese, K. Getu. Azeze, G. Asnake. Incidence and risk factors of postdural puncture headache: prospective cohort study design. Perioper Med (Lond). 2020; 9: 32. Published online 2020 Nov 9. doi: 10.1186/s13741-020-00164-2
Bodilsen, J. Mariager, T. Vestergaard, H. Højberg, M. Christiansen, M. Kunwald, M. Lüttichau, H. R. Kristensen, B. T. Bjarkam, C. R. Nielsen, H. Nielsen. Association of Lumbar Puncture With Spinal Hematoma in Patients With and Without Coagulopathy. JAMA. 2020 Oct 13;324(14):1419-1428. doi: 10.1001
Pal, A. Acharya, A. Pal, N. Dawar. Dawn, S. Biswas, J. Do pencil-point spinal needles decrease the incidence of postdural puncture headache in reality? A comparative study between pencil-point 25G Whitacre and cutting-beveled 25G Quincke spinal needles in 320 obstetric patients. Anesth Essays Res. 2011 Jul-Dec; 5(2): 162–166. doi: 10.4103/0259-1162.94757
