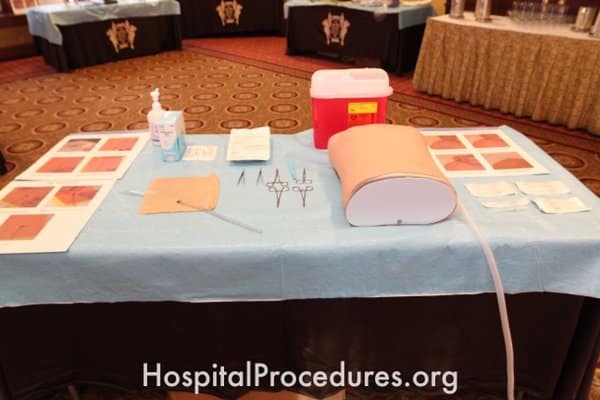
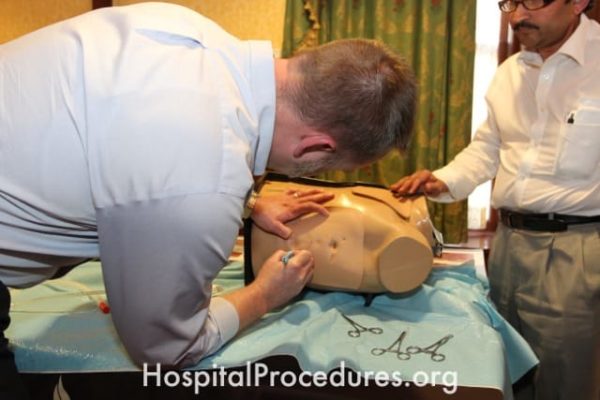
Needle decompression is indicated for the treatment of a tension pneumothorax. The needle decompression course uses an advanced simulator torso to teach needle decompression in both the mid-clavicular line or the mid-axillary line.
What you will Learn in the Needle Decompression Course
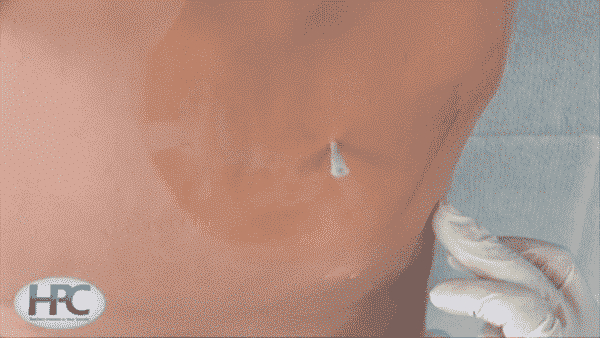
Students will learn about the release of air when the angiocatheter enters the pleural space. Needle thoracostomy is always followed by chest tube placement. Students will also learn traditional chest tube placement and wire-directed pigtail catheter placement as a part of our live CME course.
The HPC Hospitalist and Emergency Procedures course will teach you how to perform central line placement in addition to endotracheal intubation, stylet-guided intubations, laryngeal mask airway (LMA) placement, King tube placement, or fiberoptic intubations. ultrasound-guided peripheral IV access, arterial lines, POCUS exams (RUSH exams and E-FAST exams), thoracentesis, paracentesis, lumbar punctures, chest tube placement, pigtail catheter placement, needle thoracostomy, procedural sedation, and ventilator management.
Why you should choose us for your needle decompression course
Our needle thoracostomy training is a component of our live Hospitalist and Emergency Procedures CME course which teaches clinicians how to perform the 20 most essential procedures needed to work in the ER, ICU, and hospital wards.
Take your skills to the next level with our comprehensive Needle Decompression Course!
Needle Decompression Photos
More information about Needle Decompression Course
Needle decompression is a procedure used to treat patients who have a tension pneumothorax. Tension pneumothorax is when air from the lungs escapes into the pleural space – which is in between the lungs and the chest. This normally happens when the lung suffers a puncture, and when the air enters the pleural space it cannot return due to the ‘one-way-valve’ system. If enough air enters the pleural space, the lung completely collapses and the pressure in the thoracic cage prevents the heart from filling up with blood. Needle decompression is required in these circumstances as positive pressure ventilation would exacerbate this ‘one-way-valve’ effect – a buildup of pressure in the pleural space would push the mediastinum to the opposite hemithorax, which in turn obstructs venous return to the heart. This can cause many complications such as circulatory instability, which can result in traumatic arrest and can ultimately be fatal. If left untreated, tension pneumothorax can lead to cardiovascular collapse, respiratory insufficiency and even death.
There are a few causes of tension pneumothorax, the most common being blunt or penetrating chest trauma. This commonly occurs when there is a disruption of the visceral or parietal pleura, or can occasionally happen secondary to fractured ribs. Other causes can be barotrauma, central venous catheter placement, chest compressions and thoracic spine fractures. Common symptoms of tension pneumothorax vary as the condition advances. Early symptoms include chest pain, dyspnea, anxiety, tachycardia and tachypnea. If these symptoms are left to worsen, the person will display signs such as a decreased level of consciousness, hypotension, a swelling of the veins on the neck (this may not be present if hypotension has advanced) and cyanosis.
Needle decompression will quickly restore cardiopulmonary function, and reverses the physiologic effect of the tension pneumothorax. Needle decompression can indeed be life saving, however is not without its complications, so should be used by trained professionals. When administering needle decompression, the patient must first receive 100% oxygen, and must be informed to stay as still as they can. A 14 to 16 gauge angiocatheter is then inserted above the third rib in the mid-clavicular line. This is carefully administered until air can be aspirated into a syringe that is connected to a needle. If there is an immediate rush of air, this suggests a tension pneumothorax. A catheter is then advanced over the needle and left in place while a definitive chest tube is inserted on that side.
If you you would like to discuss Needle Decompression with an HPC physician we invite you to direct your question to an expert at www.Facebook.com/HospitalProcedures. We look forward to hearing from you.
Needle Decompression Course Trains Students in:
- Indications for Needle Decompression
- Contraindications to Needle Decompression
- Equipment for Needle Decompression
- Complications of Needle Decompression
- Proper positioning and technique for Needle Decompression
- Optimal sites for Needle Decompression
Needle Decompression Blogs
Basic Emergency Procedures You Should Know
What Size Catheter Should I Use For Needle Decompression For a Tension Pneumothorax?
The Reasons Hospitalists Should Learn Hospital Procedures
Survival to Hospital Discharge After Out-Of-Hospital Cardiac Arrest Is Increasing
Optimal Location for Needle Decompression For A Tension Pneumothorax
Hospitalist and Emergency Procedures CME Courses Available
Register HERE 21 days before the course to SAVE $50-150 and get the following:
- 12 month online access to Online CME course, procedure video bundle, instructional posters
- Indefinite online access to PDFs of all course lectures, course handouts, and HPC Adult Critical Care and Emergency Drug Reference Drug
Needle decompression is a life-saving maneuver performed for the stabilization of a tension pneumothorax. The needle decompression course uses an advanced simulator to teach clinicians how to perform a needle decompression in the second intercostal space of the mid-clavicular line (the proper needle decompression locations) for the treatment of a tension pneumothorax.
Our needle decompression training is a component of our live Hospitalist and Emergency Procedures CME course which teaches clinicians how to perform the 20 most essential procedures needed to work in the ER, ICU, and hospital wards.
CLICK HERE to find out more about our premier live Hospitalist and Emergency Procedures CME course
2024-08b Hospitalist and Emergency Procedures Course – San Antonio, TX (Sunday ONLY)
Courtyard Marriott San Antonio Riverwalk Hotel
November 17, 2024
Live Course & Online Course
(Sunday ONLY)
Compare Registration Types
2024-08a Hospitalist and Emergency Procedures Course – San Antonio, TX (Saturday ONLY)
Courtyard Marriott San Antonio Riverwalk Hotel
November 16, 2024
Live Course & Online Course
(Saturday ONLY)
Compare Registration Types
2024-08 Hospitalist and Emergency Procedures Course – San Antonio, TX (WEEKEND)
Courtyard Marriott San Antonio Riverwalk Hotel
November 16-17, 2024
Live Course & Online Course
(Saturday & Sunday)
Compare Registration Types
2024-07b Hospitalist and Emergency Procedures Course – New Orleans, LA (Sunday ONLY)
Intercontinental New Orleans Hotel
October 20, 2024
Live Course & Online Course
(Sunday ONLY)
Compare Registration Types
2024-07a Hospitalist and Emergency Procedures Course – New Orleans, LA (Saturday ONLY)
Intercontinental New Orleans Hotel
October 19, 2024
Live Course & Online Course
(Saturday ONLY)
Compare Registration Types
2024-07 Hospitalist and Emergency Procedures Course – New Orleans, LA (WEEKEND)
Intercontinental New Orleans Hotel
October 19-20, 2024
Live Course & Online Course
(Saturday & Sunday)
Compare Registration Types
2024-06b Hospitalist and Emergency Procedures Course – Seattle, WA (Sunday ONLY)
Crowne Plaza Seattle Downtown Hotel
September 8, 2024
Live Course & Online Course
(Sunday ONLY)
Compare Registration Types
2024-06a Hospitalist and Emergency Procedures Course – Seattle, WA (Saturday ONLY)
Crowne Plaza Seattle Downtown Hotel
September 7, 2024
Live Course & Online Course
(Saturday ONLY)
Compare Registration Types
2024-06 Hospitalist and Emergency Procedures Course – Seattle, WA (WEEKEND)
Crowne Plaza Seattle Downtown Hotel
September 7-8, 2024
Live Course & Online Course
(Saturday & Sunday)
Compare Registration Types
2024-05b Hospitalist and Emergency Procedures Course – Denver, CO (Sunday ONLY)
Sheraton Denver Downtown Hotel
July 21, 2024
Live Course & Online Course
(Sunday ONLY)
Compare Registration Types