Pericardiocentesis or a pericardial tap is a life-saving invasive medical procedure that physicians perform to eliminate a pericardial effusion, built-up fluid in the pericardium or the pericardial sac. This double-walled fibrous sac protects the heart and big vessels while supporting heart function.
Excessive pericardial fluid may lead to cardiac tamponade which causes the heart to compress and perform poorly. This medical emergency can lead to pulmonary edema (wet lung), shock, and death.
Physicians frequently perform pericardiocentesis in various settings, especially acute care environments like the emergency department (ED) and intensive care unit (ICU), among others. But this procedure is not without risks.
To avoid complications, ultrasound-guided pericardiocentesis is steadily emerging as a new way to perform a pericardial tap as it helps improve procedural safety and patient health outcomes.
Here, we take a closer look at the procedure, including why it should be the standard of care, and how it’s performed.
Ultrasound-Guided Pericardiocentesis: The New Standard of Care
Ultrasounds help diagnose pericardial effusion while determining its distribution and size. It also helps assess hemodynamic repercussions and guide pericardial taps.
Nowadays, emergency physicians commonly perform pericardiocentesis with ultrasound guidance as it has fewer complications than blind or electrocardiography-assisted procedures.
Potential complications of a pericardial tap include:
- Pneumothorax
- Right ventricular puncture
- Hepatic puncture
- Gastric puncture
- Life-threatening hemorrhage
- Infection
The growing applications of ultrasound in the emergency department (ED) have increased the viability of various techniques, including parasternal, subxiphoid, and apical, for a pericardial tap. Ultrasound guidance allows physicians to use the best technique that offers the best access to the skin’s surface where they can see the biggest fluid collection on ultrasound.
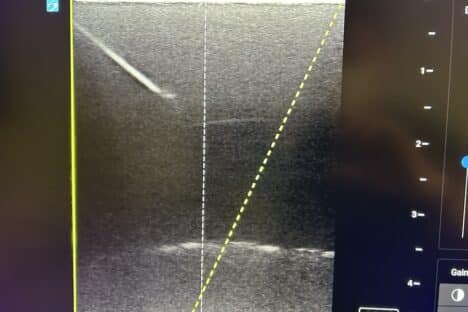
Using ultrasound imaging on the screen, clinicians can visually confirm the position of the needle tip in the pericardium and follow it while avoiding other important organs. It reduces procedural risks and improves patient safety and health outcomes.
Ultrasounds also enable quick and reliable detection of pericardial effusions which improves the effectiveness of the treatment and promotes the speedy recovery of patients.
Ultrasound-Guided Pericardiocentesis Techniques
Let us dive into the three pericardiocentesis techniques — subxiphoid, apical, and parasternal — to understand which is the best approach:
1. Subxiphoid Technique
The most common technique for a pericardial tap is the subxiphoid approach. A retrospective study on pericardiocentesis performed on patients with cardiac tamponade in the ICU found that the usage frequency of the subxiphoid technique was 99%.
But a pericardial tap’s success largely depends on the effusion’s size and distance from the skin to the pericardial fluid. Physicians must select the needle insertion site depending on where the pericardial effusion is located closest to the skin. While ultrasounds allow them to see the needle’s trajectory on a real-time basis throughout the procedure, the subxiphoid approach makes it difficult to do so.
The subxiphoid technique has the highest complication rate among the three techniques. Under this technique, the needle may penetrate and injure adjacent structures like the lungs, liver, stomach, colon, internal thoracic artery, and left anterior descending artery. It is also the farthest from the skin to the pericardium.
The subxiphoid approach is especially impractical when the fluid collection has a posterior location as it cannot reach the pericardium.
2. Apical Technique
A study by the Mayo Clinic delved into 1,127 pericardial taps performed by cardiologists in their institution over 21 years. It was found that 18% of all pericardial taps were done using the subxiphoid technique, 7% were performed from a parasternal position, and 63% were performed apically. This makes the apical approach another common pericardial tap technique.
Although the apical technique is considered better than the subxiphoid technique, it is still more difficult and less effective than the parasternal approach in most cases. Under the apical approach, it may be challenging to visualize the needle’s trajectory on a real-time basis, which may damage the adjacent structures. An apical approach also has the potential complication of pneumothorax.
3. Parasternal Technique
Recent studies have shown that the parasternal technique has lower complication rates than the subxiphoid and apical techniques for pericardiocentesis.
The parasternal approach involves laterally inserting the needle into the sternum (breastbone) on the central portion of the chest. It sonographically identifies the cardiac notch by the lack of lung tissue over the pericardium. As the pericardium is visible from the cardiac notch, clinicians can access the pericardium directly and safely.
The parasternal technique also offers a constant view of the needle tip as it advances into the body.
Also, using an in-plane parasternal medial-to-lateral technique with a high-frequency probe for pericardial tap has a much lower complication rate compared with the apical or subxiphoid approach (~2% complication rate). This technique allows physicians to visualize the needle’s trajectory and nearby vital anatomical structures better which reduces procedural risks and time.
But note that in the case of cardiac arrest, it is best to avoid the parasternal approach due to cardiopulmonary resuscitation (CPR). Instead, use the subxiphoid approach for better results. The parasternal approach may also be difficult in patients with chronic obstructive pulmonary disease (COPD) who have hyperinflated lungs as it may be difficult to get apical or parasternal views.
Currently, there are no studies that explore the most frequently used technique for ED ultrasound-guided pericardial tap. It may be because this procedure is rarely performed in emergency cases.
Conclusion
Ultrasound-guided pericardiocentesis is a reliable and safe way to perform a pericardial tap with reduced risk of complications, making it the new standard of care. Learning this technique will help clinicians improve patient care and minimize procedural time.
Our pericardiocentesis course is a fantastic way for healthcare professionals to learn all the skills and knowledge they need to successfully perform a pericardial tap. Join this course today and make ultrasound-guided pericardiocentesis part of your practice.
Resources
Willner, D. Grossman, S. Pericardiocentesis. Continuing Education Activity
Willner, D. Goyal, A. Grigorova, Y. Kiel, H. Pericardial Effusion. Continuing Education Activity
Rehman, I. Nassereddin, A. Anatomy, Thorax, Pericardium. Continuing Education Activity
Stashko, E. Meer, J. Cardiac Tamponade. Continuing Education Activity
Blanco, P. Figueroa, L. Menendez, M. Pericardiocentesis: ultrasound guidance is essential. Ultrasound J. 2022; 14: 9. 10.1186/s13089
Stolz, L. Situ-LaCasse, E. Acuña, J. Thompson, M. What is the ideal approach for emergent pericardiocentesis using point-of-care ultrasound guidance?. World J Emerg Med. 2021; 12(3): 169–173
Vayre, F. Pezzano, L. Subxiphoid pericardiocentesis guided by contrast two-dimensional echocardiography in cardiac tamponade: experience of 110 consecutive patients. Eur J Echocardiogr. 2000;1(1):66-71. doi: 10.1053/euje.1999.0003.
Osman, A. Chuan, T. Rahman, J. Ultrasound-guided pericardiocentesis: a novel parasternal approach. Eur J Emerg Med. 2018; 25(5): 322–327
