Intraosseous lines are commonly associated with decreased return of spontaneous circulation or ROSC rates compared to peripheral IV access. Intraosseous lines have also been linked to decreased survival after out-of-hospital and in-hospital cases of cardiac arrest in comparison to IV resuscitation. But is this actually the case?
How Intraosseous Lines Work
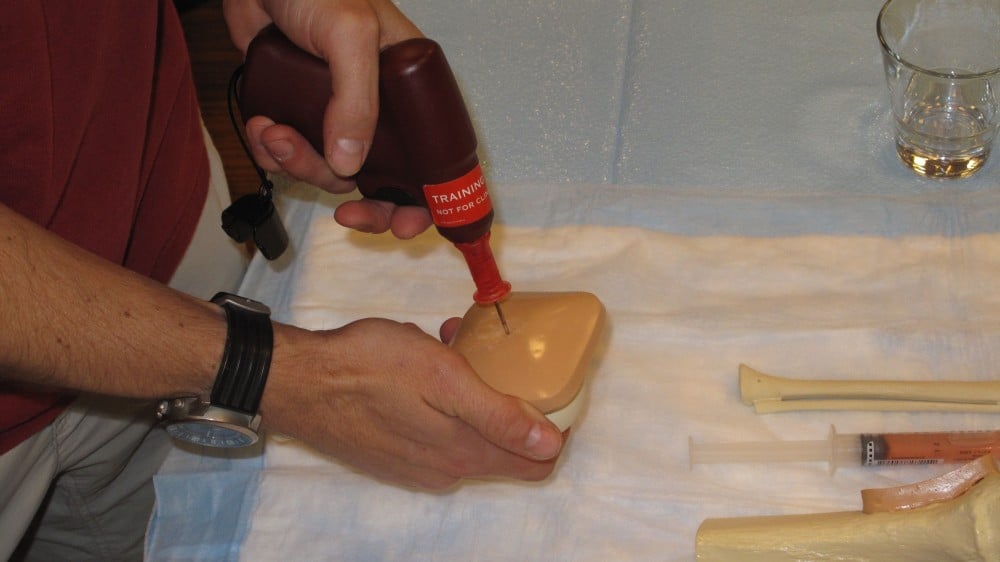
Intraosseous lines are an alternative way of administering life-saving description drugs when venous catheterization is currently not possible. Otherwise called intraosseous access, it is generally used as a short-term vascular access solution that stabilizes the patient in emergency situations within and outside the hospital setting. It has a maximum 24-hour allowable duration when used for emergent patients.
Intraosseous access could be a viable option when the blood vessels collapse. In other words, when vascular access becomes a major challenge in medical emergencies, the bone marrow can serve as a non-collapsible vein for medicine administration. Moreover, IO insertion into the bone is relatively quicker and easier to locate than blood vessels.
Why do people opt for intraosseous lines?
Venous access is oftentimes one of the greatest challenges when it comes to emergency situations and critically ill patients. The peripheral veins become difficult to cannulate and the blood vessels collapse, making it difficult to use intravenous solutions during medical emergencies. Because of this, intraosseous infusion was developed as a quick, safe, and reliable way to get emergency venous access for a maximum of 24 hours.
The bone marrow space essentially serves as a non-collapsible vessel that provides access to the vascular system. As such, even though fluids and medications can’t be administered via IV because of collapsed veins, they can still enter the system.
Here, we reiterate that the use of intraosseous lines isn’t so much a choice. Rather, it becomes a necessity due to the surrounding circumstances of a medical emergency.
When does intraosseous access become necessary?
Intraosseous lines offer an alternative to IV when emergency fluids and medications need to be distributed within the system as quickly as possible. It becomes necessary when conventional peripheral IV access becomes too difficult. As such, it might be an option for cases of burns, shock, status epilepticus, and cardiopulmonary arrest.
During cardiopulmonary arrest and the other aforementioned situations, there are usually attempts at administering fluids and medication through peripheral IV lines first before making the decision to use intraosseous access.
Intraosseous lines are used in hospital cases of cardiac arrest and severe shock. Intraosseous access can also be used during pre-hospital critical care transport.
Is intraosseous access safe for all patients?
Although intraosseous lines are an option in situations of cardiac arrest and severe shock, it is not always recommended.
Patients with fractured bones or with previously punctured bones should not undergo intraosseous infusion because the fluid will likely extravasate, lead to compartment syndrome, and cause further complications. In this case, it’s important to first check for alternate bone sites before proceeding.
It’s also best to get a second opinion before proceeding with intraosseous infusion if the patient has osteopetrosis, osteogenesis imperfecta, or other bone diseases as the conditions could interfere with the infusion.
How Intraosseous Lines Compare to Peripheral IV Access
Given sufficient background information about intraosseous lines, we’ll now dive into how they’re different from peripheral IV access. After all, intraosseous access has been associated with lower ROSC during chest compression and, subsequently, patient survival rates after in-hospital cardiac arrests in comparison to IV.
This is something that Kevin T. Schwalbach, Sylvia S. Yong, R. Chad Wade, and Joseph Barney tackled in a retrospective study that was published online in 2021. Among 1039 eligible subjects, they noted that 832 patients were resuscitated with the help of peripheral IV access. Meanwhile, 207 patients survived via intraosseous lines.
Is there really a higher chance of survival with peripheral IV?
Although the numbers say that 832 out of the 1039 eligible research subjects survived in-hospital cardiac arrest because of peripheral IV, it doesn’t automatically imply that IV access is more effective than intraosseous lines — we have to take other factors and individual circumstances into consideration as well. The rest of the numbers say:
- The study showed a 20.8% use of intraosseous access, compared to the notable higher use of peripheral IV which was 28.4% in total.
- Cardiac arrest survival rates that have favorable neurologic status was 18.4% for intraosseous and 25.2% for peripheral IV lines.
- Intraosseous access had a longer TTR of 12:38 minutes on average compared to the 9:01-minute average of peripheral IV access.
- Patients who were resuscitated with the help of intraosseous lines had an 80.2% likelihood of a witnessed arrest, while it’s 86.5% for peripheral IV.
- Intraosseous access results in a 3:06-minute time-to-epinephrine average, while the peripheral IV route had a 2:32-minute average.
It seems like peripheral IV is safer and more effective for cardiac arrest patients. However, when the variants were adjusted to provide a more equal outlook of the results, the numbers showed no significant difference between the survival rates in relation to intraosseous lines and peripheral IV access. The only real noticeable difference lies in the TTR, which is significantly longer for the intraosseous group.
That being said, there’s no real harm or benefit of using intraosseous lines peripheral IV or the other way around. Intraosseous access may be associated with lower ROSC times and survival rates. But in total, they are relatively on the level with peripheral IV.
As medical research continues to advance, we will eventually have in-depth knowledge of the matter.
References
Schwalbach, K. Yong,S . Wade, R. Barney, J. Impact of Intraosseous Versus Intravenous Resuscitation During In-Hospital Cardiac Arrest: A Retrospective Study. Resuscitation. 2021. 166: 7-13.
Garner, L. Complications and circumstances pertaining to intraosseous lines. Health Policy and Services Research. 2016 (9)
Dornhofer, P. Kellar, J. Intraosseous Vascular Access. Continuing Education Activity. 2022 (6)
Torlincasi, A, Lopez, R. Wassem, M. Acute Compartment Syndrome. Continuing Education Activity. 2022 (8)
