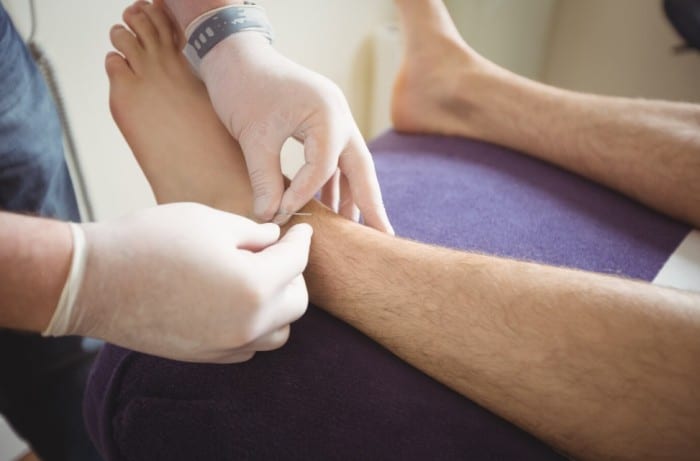
Though initially performed in the resuscitation of pediatric patients, it has now become a safe and reliable alternative for all time-sensitive situations. Multiple studies have shown that it is a quick and reliable option to take samples for point-of-care (POC) analysis to guide clinical decision-making and ensure better outcomes.
Understanding Intraosseous Line Insertion
Intraosseous line insertion in healthcare refers to the placement of a hollow bore needle to deliver emergency drugs. It is twice as likely to be successful than peripheral IVs, provides access within 20 seconds, and is safe for all age groups, including compromised neonates. There are no long-term side effects, which should make it the first option when IV access is not available.
IO access can be used to deliver the following: adenosine, amiodarone, atropine, cisatracurium, dobutamine, dopamine, epinephrine, etomidate, heparin, insulin, lidocaine, morphine, norepinephrine, propofol and all ACLS medications.
It can also be used for:
- Contrast products.
- Resuscitative fluids (crystalloids, colloids, Ringer’s lactate)
- Blood products (red blood cells, platelets, fresh frozen plasma)
IO aspiration of blood can also be used for laboratory tests, such as hemoglobin and hematocrit levels. However, since lactate and glucose values vary, as do potassium, it’s important to repeat tests with IV access for accurate results.
Common Sites for Intraosseous Access
Potential sites for IO access include the sternum, distal tibia, proximal tibia, and proximal humerus —the last three are the ideal options for adults. and infants.
It’s important to palpate both borders of the site before inserting the needle to ensure central penetration.
Indications
Intraosseous access is indicated for patients who need immediate IV fluids or medication, but conventional peripheral or central IV access is not feasible, has failed, or is difficult to obtain. It is critical in extreme conditions like search and rescue.
Some scenarios where it is an acceptable route to minimize morbidity and mortality include, but are not limited to:
- Sepsis
- Shock
- Trauma
- Poisoning
- Hypovolemia
- Severe edema
- Cardiac arrest
- Severe bleeding
- Extensive burns
- Status epilepticus
- Severe dehydration
If the patient is conscious, local anesthesia should be used through the IO needle after insertion.
Contraindications
Contraindications for Intraosseous line insertion include:
- Burns
- Cellulitis
- Osteomyelitis
- Coagulopathies
- Previous IO access
- Ipsilateral fractures
- Osteoporosis (relative)
- Local vascular injuries
- Compartment syndrome
- Osteogenesis imperfecta
- Fracture of the target bone
- Infection at the puncture area
- Attempted IO access in target bone within 48 hours
- Prosthesis or recent orthopedic procedure near the insertion site
It also includes an inability to accurately identify landmarks at the chosen site.
What Equipment is Required?
These devices can be used for Intraosseous line insertion in healthcare:
- Manual IO needles with a central removal stylet (Dieckmann modified needle, Jamshidi needle)
- Mechanical IO devices (BIG (bone injection gun), arrow EZ-IO®, FAST1™ intraosseous infusion system, and NIO (new intraosseous) device)
These have similar applications and techniques for insertion, but some are more suited for specific puncture sites than others.
The proximal tibia is the recommended insertion site with a mechanical device—it is flat, easy to locate, and has a thin layer of tissue over the bone. For sternal sites, FAST1 is recommended to avoid penetration into the thoracic aorta.
The distal tibia is preferred for a manual approach: its thin bone cortex makes insertion easier.
Manual Intraosseous Line Insertion Technique
Stabilize the leg and clean the injection site. Place the single-use needle perpendicular to the long axis of the bone. The right size depends on weight, accounting for site anatomy and tissue depth (25mm 15-G for patients weighing 3 kg or more, 15mm 15-G for 3 to 39 kg, and 45mm 15-G for above 40 kg or those with excessive tissue depth).
Apply minimal pressure until you feel a hard stop, indicating the needle has touched the bone. At least 5 mm of the needle must be visible above the skin to confirm penetration into the medullary space.
Next, inject 1-2% IV lidocaine for pain relief and allow for 120 seconds to take effect. Flush with normal saline (5 to 10 cc for adults and 2 to 5 ml for infants and children) for confirmation of placement.
Secure the tubing with tape and immobilize the leg until the catheter is removed to prevent dislodgement. Document the date and time of insertion—it must be removed within 24 hours to minimize the risk of complications.
Possible Complications
While intraosseous line insertion in emergency healthcare is a relatively safe procedure, complications can still occur even after needle placement.
Misplacement could lead to extravasation of fluid, which can cause localized tissue necrosis. It has also been associated with compartment syndrome of the leg, iatrogenic fractures, injury to growth plates, soft tissue complications, and cellulitis. And, in one rare case, thrombosis. For pediatric patients, there is a risk of epiphyseal plate necrosis.
That said, the incidence of complications is rare, at 0.9%.
Enhance Outcomes with Hospital Procedures
IO placement is considerably faster than central lines and US IV, but this life-saving technique is underutilized despite recommendations from advanced trauma and cardiac life support guidelines. This could be down to a lack of physician confidence with IO access.
Training with an intraosseous line course with Hospital Procedures Consultants is needed to learn everything about this valuable technique.
Resources
Tsotsolis,N. Tsirgogianni, K. Kioumis, I. Pitsiou, G. Baka, S. Papaiwannou, A. Karavergou, A. Rapti, A. Trakada, G. Katsikogiannis, N. Tsakiridis, K. Karapantzos, I. Karapantzou, C. Barbetakis, N. Zissimopoulos, A. Kuhajda, I. Andjelkovic, D. Zaragoulidis, K. Zaragoulidis, P. Pneumothorax as a complication of central venous catheter insertion. Ann Transl Med. 2015 Mar; 3(3): 40. Doi: 10.3978/j.issn.2305-5839.2015.02.11
Jousi, M. Bjorkman, J. Nurmi, J. Point-of-care analyses of blood samples from intraosseous access in pre-hospital critical care. Acta Anaesthesiol Scand
. 2019 Nov;63(10):1419-1425. doi: 10.1111/aas.13443. Epub 2019 Jul 23.
Shelly,P. Raluca, A. Stefan, M. Tomas Saund, Lee, S. Insertion of an Intraosseous Needle in Adults. CME
Strandberg, G. Larsson, A. Lipcsey, M. Eriksson, M. Comparison of Intraosseous, Arterial, and Venous Blood Sampling for Laboratory Analysis in Hemorrhagic Shock. Clin Lab. 2019 Jul 1;65(7). doi: 10.7754/Clin.Lab.2019.181214.
Miller, L. Philbeck, T. Montez, D. Spadaccini, C. A new study of intraosseous blood for laboratory analysis. Arch Pathol Lab Med. 2010 Sep;134(9):1253-60. doi: 10.5858/2009-0381-OA.1
Ellemunter, H. Simma, B. Trawoger, R. Maurer, H. Intraosseous lines in preterm and full term neonates. Arch Dis Child Fetal Neonatal Ed. 1999 Jan; 80(1): F74–F75.
doi: 10.1136/fn.80.1.f74
Dornhofer, P. Kellar, J. Intraosseous Vascular Access. StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan. 2023 Jun 5
Chreiman, K. Dumas, R. Seamon, M. Kim, P. Reilly, P. Kaplan, L. Christie, J. Holena, D. THE IOs HAVE IT: A PROSPECTIVE OBSERVATIONAL STUDY OF VASCULAR ACCESS SUCCESS RATES IN PATIENTS IN EXTREMIS USING VIDEO REVIEW. J Trauma Acute Care Surg. Author manuscript; available in PMC 2019 Apr 1
