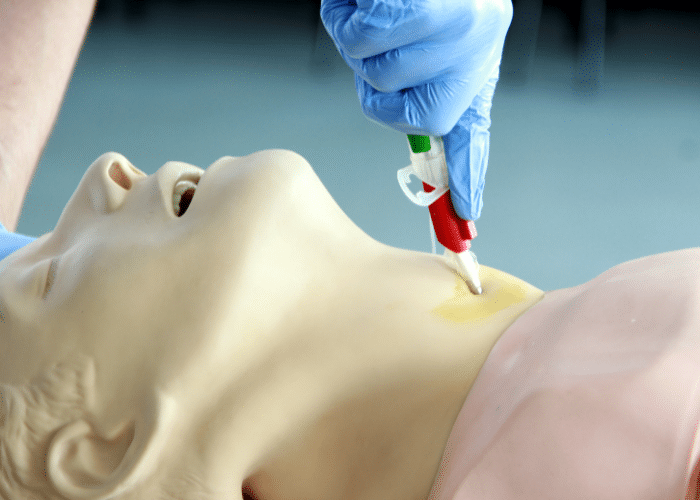
However, “cannot intubate, cannot ventilate” (CICV) scenarios that require FONA must be resolved within a few minutes to achieve a favorable outcome. Failing to successfully perform the procedure promptly could lead to serious consequences like hypoxic brain injury and even death.
Join Hospital Procedures Consultants as we review emergency airway techniques like front-of-neck access, including its two techniques: cricothyroidotomy vs tracheostomy.
Importance of FONA
When clinicians are unable to access a patient’s airway with face mask ventilation, tracheal intubation, or a supraglottic airway device, there is a significant risk of hypoxia (a form of oxygen deficiency).
Death and brain damage are also known to occur in one out of 180,000 patients. If the first airway intervention fails to deliver the desired results in the ED or ICU, it could lead to cardiac arrest and even death after hypoxia within 45 to 60 minutes.
FONA is thus the last resort during life-or-death situations. Though important, it is associated with several adverse events which could be caused by the misplacement of the intubation tube cephalad, one-lung intubation, hemorrhage requiring hemostasis, cuff injury, mediastinal/subcutaneous emphysema, pneumothorax, and poor ventilation due to tube kink.
Choosing the right technique can significantly improve patient outcomes.
Techniques for CICV Situations
There are two main techniques to assess the airway in emergency CICV scenarios:
- Cricothyroidotomy (performed with a scalpel or cannula)
- Surgical tracheostomy
The Difficult Airway Society recommends cricothyroidotomy with a scalpel-bougie-tube as a first line technique for emergency FONA.
It is fast and reliable, with a 100% success rate within two attempts. Cricothyroidotomy is thus typically used due to the risk of aerosolization with the oxygen insufflation associated with the cannula.
This is because cannula cricothyroidotomy calls for inserting a small or large caliber cannula percutaneously to facilitate ventilation. It fails 63% of the time when a narrow bore cannula is used, though a kink-resistant cannula could reduce the high incidence of failure. It demonstrates similar outcomes in 43% of cases where the wide bore technique is used.
There has been a lot of debate on whether a scalpel or cannula is better for this technique. They have varying results due to the use of manikin and cadavers that do not truly replicate human patient characteristics. Hence, instead of worrying about the optimal technique, the focus should be on a wider human factors approach.
If a cricothyroidotomy were to fail, an emergency tracheostomy should be used as a rescue intervention. However, it’s important to note that tracheostomy tube insertion can be rapidly fatal. Due to the increased risk of complications, it must only be performed by experienced professionals.
A Look at the Performance of Emergency FONA Access by Different Surgical Departments
A 2019 study by Groom and colleagues timed 3 phases for eFONA:
Deliberation Time
Recording the onset of CICV starting FONA, revealed no significant differences between the three groups in this category. Anesthetists, head and neck surgeons, and general surgeons respectively took 30, 31, and 23 seconds to decide on emergency surgical FONA.
Surgical Time
Surgical time was recorded from the start to finish of FONA, with a confirmation of chest expansion after intubation. Anesthetists took a median of 50 seconds to complete the procedure while head and neck surgeons took 74 seconds and general surgeons took 86 seconds.
Total Time
Total time refers to when anesthetists declared a CICV situation due to their inability to oxygenate the patient up until the completion of the surgical FONA.
There was no significant difference in total time across the three groups. Anesthetists took a median time of 86 seconds to complete the procedure, head and neck surgeons took 98 seconds, and general surgeons took 126 seconds.
Who Should Administer FONA?
Rescuing the airway via the neck falls under Plan D in the DAS Difficult intubation guidelines. It is a challenging, time-sensitive procedure that requires advanced non-technical and psychological skills, which many medical practitioners lack. Hence, it is often performed too late or not at all.
This reluctance is a major contributor to morbidity and mortality in CICV. This is why a “double setup airway intervention” is commonly suggested.
As demonstrated by the comparative study highlighted in the previous section, CICO doesn’t have to be reliant on head and neck surgeons. In emergency situations, surgical FONA can also be performed by properly trained anesthetists.
Groom and colleagues looked at performance in a simulated scenario, using a manikin to simulate a patient’s prosthetic bleeding. This was probably because research is restricted due to ethical considerations.
They highlighted the importance of a multidisciplinary team that employs a shared “deliberate practice.” Per a 2019 study, they must be able to reduce deliberation time, procedural time, and “lost time” spent managing a CICV situation while minimizing the risks of cerebral and cardiac hypoxia.
Combining Strategies
The second and third interspaces in tracheal rings are commonly used for tracheostomy, but overlying anatomical variations—like major vessels anterior to the trachea, above the suprasternal notch—can cause difficulty.
Because of this, it would be worthwhile to pair eFONA with ultrasonography to localize the essential cricothyroid membrane and tracheal rings.
Without proper identification of the cricothyroid membrane (CTM), there is a risk of tube misplacement, leading to a failed cricothyroidotomy. In CICV situations, there is also a risk of damaging local structures, which can cause tension in the pneumothorax, pneumomediastinum, and mediastinitis.
If the equipment isn’t available, conventional palpation may be used to identify the CTM. This method has been successful in 40% to 70% of patients based on body habitus.
Learn Skills for Cricothyroidotomy vs Tracheostomy at HPC
An emergency front-of-neck airway isn’t just relevant in situations where the primary airway interventions fail. Cricothyroidotomy vs tracheostomy can also be used to secure the native upper airway from advanced head and neck tumors as well as traumatic injuries to the face and neck.
Since poor training and experience are primary drivers of serious airway events, it’s important to get regular training to improve health outcomes.
Hospital Procedures Consultants offer airway management courses that take you through the basic techniques and provide insights into emergency cricothyrotomy in challenging CICO situations. To learn more, please visit our website.
Resources
Greenland, K. B. Sommerville, R. S. Emergency front-of-neck airway: strategies for addressing its urgency. Br J Anaesth. 2019 Nov;123(5):545-548. Doi: 10.1016/j.bja.2019.08.008. Epub 2019 Sep 18
Okada, A. Okada, Y., Kandori, K. Ishii, W. Narumiya, H. Iizuka, R. Adverse events of emergency surgical front of neck airway access: an observational descriptive study. Acute Med Surg. 2022 Apr 15;9(1):e750. doi: 10.1002/ams2.750. eCollection 2022 Jan-Dec
Price, T. M. McCoy, E. P. Emergency front of neck access in airway management. BJA Educ. 2019 Aug; 19(8): 246–253.
McKenna, P. Desai, N. M. Tariq, A. Morley, E. J. Cricothyrotomy. Book.
