Indications for a Thoracentesis
THORACENTESIS COURSE - cont'd info
Indications for Thoracentesis
Diagnostic
– Work-up unexplained pleural effusion
– Rule out empyema
Therapeutic
To relieve dyspnea and improve oxygenation
Contraindications for a Thoracentesis
Contraindictations
Absolute Contraindications
– Uncooperative patient
– Overlying skin infection
– Ruptured diaphragm
Relative Contraindications
– Small pleural effusion (≤ 1 cm on lat decubitus CXR)
– Loculated effusion
– Mechanical ventilation
– Coagulopathy (INR > 2.5 or PTT > 1.5 x upper limit NL)
– Thrombocytopenia (Platelets < 25K)
– Thienopyridine antiplatelet or DOAC use
– Severe uremia
Complications of a Thoracentesis
Complications of Thoracentesis
Pheumothorax (incidence 1- 2% overall)
– Tube thoracostomy if symptomatic or > 15%
– 1/3 of all pneumothoraces require a chest tube
Risk factors for pneumothorax
– Inexperienced operator (3.9% vs 8.5%)
– Therapeutic thoracentesis (OR 2.5)
– Mechanical ventilation (OR4, NS)
– >2 attempts (OR 2.5, NS)
Minimize risk with ultrasound- guidance (OR 0.3)
– Manual aspiration
Re expansion pulmonary edema (0.5 %risk)
– Unlikely by limiting to removal of 1.5 L pleural fluid
– Avoid suction against excessive negative pressure
Local infection (1% risk)
Laceration of intercostal artery causing a
hemothorax (1.2%)
Shearing of the catheter
Injury to spleen, liver, diaphragm or lung
– Avoid entry sites below 8th ICS in midscapular line
Equipment for a Thoracentesis
Proper positioning and technique for a Thoracentesis
- The patient is placed in a sitting position with the arms resting on a table placed in front of the patient
- The thoracentesis is performed along the posterior thorax
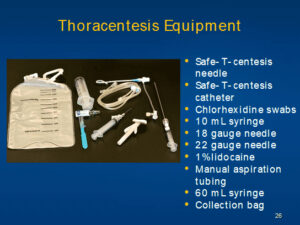
Thoracentesis Equipment
- Safe-T-centesis needle
- Safe-T-centesis catheter
- Chlorhexidine swabs
- 10 mL syringe
- 18 gauge needle
- 22 gauge needle
- 1% lidocaine
- Manual aspiration tubing
- 60 m L syringe
- Collection bag
Technique
- Informed Consent
- Percuss out superior margin of effusion or identify optimal site with ultrasound
- Insertion site should be at least 6 cm lateral to spine
- Perform a “Time out” and mark site after rechecking a chest ×-ray to confirm correct side
- Anesthetize skin, periosteum and pleura over rib
- Advance 1.5 inch 22 gauge finder needle with constant aspiration until fluid return
- Memorize depth required to enter pleural space
- Advance thoracentesis needle until pleural fluid is aspirated
- Once fluid returns, advance catheter to appropriate depth of insertion
- Withdraw needle out of skin and leave catheter in place
- Manual aspiration using 3-way stopcock for therapeutic thoracentesis
-
- Stop aspiration for worsening dyspnea, severe chest pain, intractable coughing or sentation of increased negative pressure
- Lower risk of REPE and pneumothorax with manual aspiration vs vacuum cannisters
Ultrasound-directed Thoracentesis
Ultrasound used to identify the optimal insertion location and then the patient is kept in the same position and the skin is then prepped with chlorhexidine and sterile drape applied
Ultrasound for Pleural Effusion
- Use a convex array 3.5-5 MHz probe
- Direct groove cephalad
- Identifv location of diaphragm
- Identify the best fluid pocket and mark with a pen
- Perform thoracentesis with pt in same position
- Success rate is 95% with ultrasound guidance
- Increased rate of accurate site selection by 26%
- Fluid can be successfully obtained in 85% of patients
after unsuccessful blind thoracentesis
Pleural fluid analysis
Ultrasound used to identify the optimal insertion location and then the patient is kept in the same position and the skin is then prepped with chlorhexidine and sterile drape applied
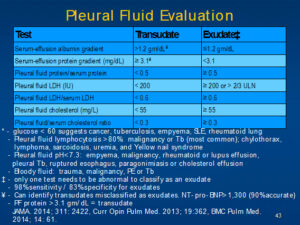
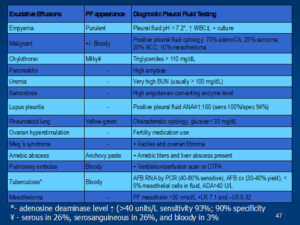
Pleural Fluid Evaluation
– Glucose < 60 suggests cancer, tuberculosis, empyema, SLE rheumatoid lung Pleural fluid lymphocytosis >80% malignancy or Tb (most common); chylothorax,lymphoma, sarcoidosis, uremia, and Yellow nail syndrome
– Pleural fluid pH<7.3: empyema, malignancy, rheumatoid or lupus effusion, pleural Tb, ruptured esophagus, paragonimiasis or cholesterol effusion
– Bloody fluid: trauma, malignancy, PE or Tb
– only one test needs to be abnormal to classify as an exudate
– 98% sensitivity / 83% specificity for exudates
– *Can identify transudates misclassified as exudates. NT- pro- ENP> 1,300 (90%accurate)
– PF protein > 3.1 gm/ dL = transudate
Transudative Effusions
Common Causes
– Congestive Heart Failure*
– Hepatic hydrothorax* (13- 16 %incidence of spontaneous bacterial empyema)
– Nephrotic syndrome*
– Severe hypoalbuminemia*
– Trapped lung
Uncommon Causes
– Constrictive pericarditis
– Peritoneal dialysis
– Superior vena cava syndrome
– Urinothorax
– Myxedema
Coding for a Thoracentesis
Coding for a Thoracentesis
- 32554 Thoracentesis without image guidance
- 32555 Thoracentesis with image guidance
-52 Procedures that are incomplete or discontinued at physician’s discretion
-53 Procedures that are discontinued because the patient’s life is endangered