PROCEDURAL SEDATION COURSE - cont'd info
Informed Consent
- Informed consent is founded on a patient’s right to autonomy and self-determination
- Healthcare provider must establish that the patient has decision-making capacity for the patient to be able to provide informed consent for him/herself
- The patient must display the following to demonstrate decision-making capacity
– Understand their medical diagnosis
– Understand the benefits of having the procedure
– Understand the potential complications of the procedure
– Understand the probable outcomes of declining the procedure
- Informed consent involves a discussion between the physician and patient covering
– Procedural benefits
– Procedural complications
– Potential alternatives
– Potential outcomes of not having the procedure
– Patient must be able to recite back to clinician the benefits of having the procedure, potential complications and probable outcome of declining the procedure
- By definition, incompetent or incapacitated adults may not provide informed consent for any procedure. A surrogate decision maker would need to provide informed consent on behalf of an incompetent or incapacitated adults
- In general, minors (<18 years old) cannot provide informed consent for a bedside medical procedure unless they are an emancipated minor
- In many states, minors over the age of 14 years may obtain certain services without parental consent. These services include birth control, sexually transmitted disease therapy (including HIV therapy), immunizations, prenatal care, mental health services, substance abuse services and possibly abortion services WITHOUT parental consent
Indications for Procedural Sedation
Procedural Sedation
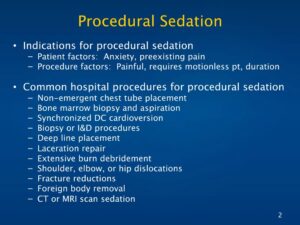
Indications for procedural sedation
– Patient factors: Anxiety, preexisting pain
– Procedure factors: Painful, requires motionless pt, duration
Common hospital procedures for procedural sedation
– Non-emergent chest tube placement
– Bone marrow biopsy and aspiration
– Synchronized DC cardioversion
– Biopsy or I&D procedures
– Deep line placement
– Laceration repair
– Extensive burn debridement
– Shoulder, elbow, or hip dislocations
– Fracture reductions
– Foreign body removal
CT or MRI scan sedation
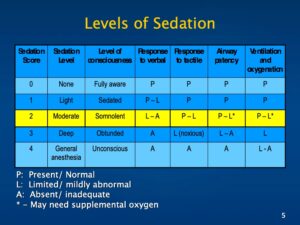
Levels of Procedural Sedation

Airway Assessment
Airway examination
- Assess Mallampati class airway
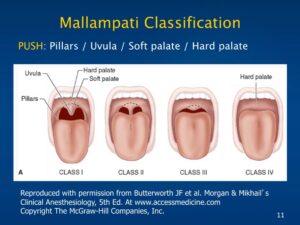
- Assess neck extension (≥ 70 degrees is normal)
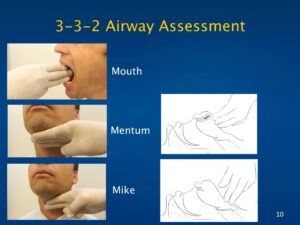
- 332 rule (“Mouth, Mentum, Mike”)
– 3 finger widths between teeth with mouth wide open
– Chin length at least 3 finger widths (Hyomental distance)
– Thyromental distance at least 2 finger widths
Examination Findings Predicting a Difficult Airway
- High arched palate
- Low set ears
- Thick short neck
- Marked facial distortion
- Prior radiation therapy to the neck or oropharynx
- Neck mass
- Facial trauma
- Macroglossia
- Small mandible
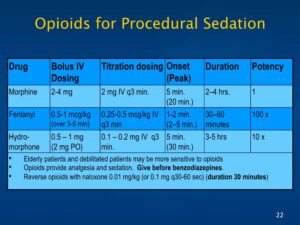
Opioids for Procedural Sedation
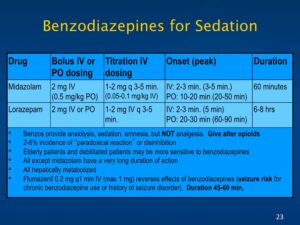
Benzodiazepines for Procedural Sedation
Ketamine for Procedural Sedation

Ketamine
Premedication (in adults)
- Midazolam (0.03 mg/kg, max 2 mg) IV minimizes
emergence reactions - “Set the dream”
Dosing (Dissociative State)
- 1-1.5 mg/kg (adults) or 1.5-2 mg/kg (children) IV or
3-4 mg/kg IM (children) - May give additional 0.5-1 mg/kg IV (max 2 mg/kg)
Onset (Duration)
- IV=1-2 min (20-30 min)/IM=2-10 min (80-120 min)
Benefits
- amnesia, sedation, analgesia and bronchodilation
- NO RISK OF RESPIRATORY DEPRESSION
Side Effects
- hypersalivation, BP ↑, HR ↑, vomiting (6-8%)
emergence reactions (up to 50% adults, 6-8%
children), ↑ I0P, myoclonic jerks
Propofol for Procedural Sedation

Propofol "Milk of amnesia"
Dosing
- Bolus IV dosing: 1 mg/kg IV bolus then 0.5 mg/kg IV
q3 min prn - Titration dosing: 20 mg IV q 30-60 seconds to affect
- Typical dose 1-1.5 mg/kg IV (0.75-1 mg/kg IV in elderly)
- Onset (duration): 1 minute (5-10 minutes)
- Adjunctive meds: fentanyl 0.5 mcg/kg IV PRIOR to propofol
- Avoid with an egg/soy allergy
- Caution in children with mitochondrial disorders
- Benefits: ↓ ICP, bronchodilates, antiemetic and anticonvulsant
- Drawbacks: ↓ BP, resp. depression (3-9%), tremors, NO
ANALGESIA
Ketofol for Procedural Sedation
"Ketofol"
Titration dosing
– 1:1 mixture of ketamine (10 mg/mL) and
propofol (10 mg/mL)
– 2-3 mL IV q30-60 sec titrated to effect
Bolus dosing
– 0.75 mg/kg IV ketamine over 1-2 minutes
– 0.75 mg/kg IV propofol over 1 minute
Benefits: Less hypotension; less apnea
Drawbacks: hypersalivation, BP ↑, HR ↑,
vomiting (6-8%), emergence reactions,
and increased intraocular pressure
Etomidate for Procedural Sedation

Etomidate
Dosing
> Initial dose: 0.1 mg/kg IV bolus
> Titration dosing: 0.05 mg/kg IV q3-5 min to affect
> Max for sedation: 0.2 mg/kg
– Onset (duration): 1 minute (5-15 min)
– Adjunctive meds: Give IV opiates PRIOR to etomidate
– Benefits: no hemodynamic effects, decreases ICP and
spontaneous respirations usually maintained (10%
risk of apnea)
Side effects:
>Vomiting (WATCH AIRWAY)
> Myoclonus (20-45%)
> NO ANALGESIA
> Adrenal suppression (biochemical)
Topical Anesthetics for Analgesia in Children

Topical Anesthetics
EMLA cream (Eutectic mixture of local aesthetics
with 2.5% lidocaine and 2.5% prilocaine)
– Indications: IV cannulation, venipunctures or lumbar punctures
– Advantages: painless application
– Disadvantages: must wait 60 minutes for peak effect and must be applied to intact skin
LET cream (lidocaine, epinephrine and tetracaine)
– 15 mL 2% viscous lidocaine: 7.5 mL topical epinephrine 1:1000; 7.5 mL 2% topical tetracaine
– Indications: laceration repair
– Advantages: can be applied to nonintact skin
– Onset of action: 20 minutes
Coding for Procedural Sedation

Coding for Procedural Sedation
- 99143 Moderate procedural sedation provided by same physician
performing diagnostic or therapeutic procedure
– age <5, first 30 min - 99144 Moderate procedural sedation provided by same physician
performing diagnostic or therapeutic procedure
– age> 5, first 30 min - 99145 Each additional 15 min
- 99148 Moderate procedural sedation provided by a different
physician other than procedural physician
– age <5, first 30 min - 99149 Moderate procedural sedation provided by a different
physician other than procedural physician
– age>5, first 30 min - 99150 Each additional 15 min
- 36000 Introduction of intravenous needle or catheter
