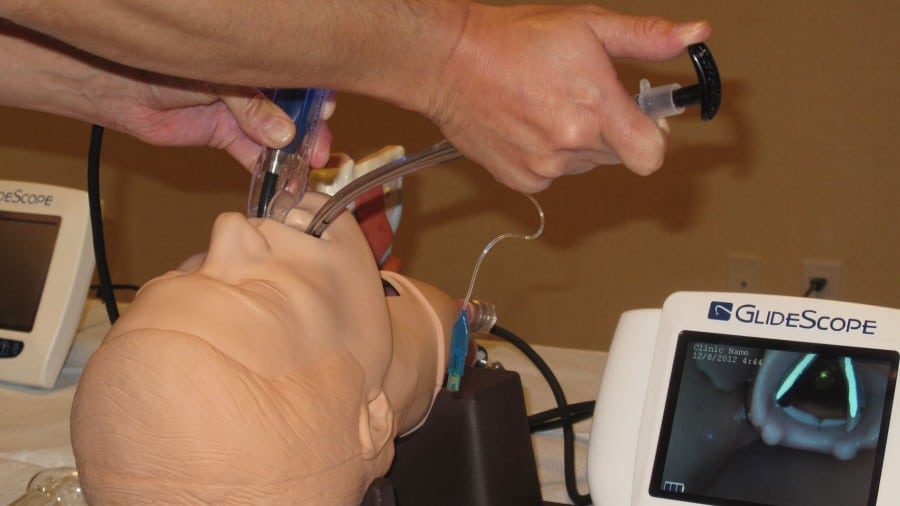
Videolaryngoscopy has quickly become a popular method for airway management because it provides better visuals of the glottis. Failed intubations have decreased since more clinicians have begun to rely on videolaryngoscopy and the greater visibility it provides.
Awake videolaryngoscopy is proving to be a superior method. Many patients prefer to be asleep during medical procedures like videolaryngoscopy but there is one great advantage when the patient is awake — they have agency over their airways. The operator can easily communicate with them while the procedure is ongoing.
There is thus a greater margin of safety when general anesthesia is omitted from the procedure and the patient remains conscious.
Until recently, awake fibreoptic intubation (FOI) has been the common option for the management of anticipated difficult airways. However, in recent years, medical experts have rallied behind awake videolaryngoscopy because it is much easier to perform.
How Is Awake Videolaryngoscopy Done?
To prepare a patient for awake videolaryngoscopy, the airway is dried. To do this, intravenous or intramuscular desiccants, suction, gauze sponging, or a combination of these methods are used.
More often, topical anesthesia is required. Any sedation administered must be a modest amount to keep the patient awake and cooperative. Patients are asked to open their mouths and extend their tongues as the videolaryngoscope is slowly inserted.
The videolaryngoscopy operator will ensure that the device is not touching the posterior pharyngeal wall as it may induce a gag reflex. In case there is a gag reflex, an additional topical anesthetic will be administered through an atomizer or spray.
Who Needs Awake Videolaryngoscopy?
People who have difficulty breathing can receive help through machines. They need to be intubated to open up the airway while the machine delivers air or oxygen into the body.
During the intubation process, a tube is inserted into the patient’s mouth or nose which then makes its way down to the trachea so the passage is kept open for oxygen. The laryngoscope guides the endotracheal tube during intubation.
Direct laryngoscopy was developed to establish visualization of the larynx. The ability to see is important in hospital settings for eventual tracheal intubation.
Using a high-resolution micro camera, videolaryngoscopy provides better visuals that improve the success rate of tracheal intubation. The goal among healthcare practitioners is to achieve intubation success on the first attempt.
Who Needs Intubation?
Anyone who has difficulty breathing or experiences problems getting oxygen into their system needs to be intubated. These specific cases require intubation:
- Cardiac arrest – oxygen levels decrease during cardiac arrest or the sudden loss of heart function
- Injury – some injuries, especially those that affect the abdomen, chest, or neck, could affect the airway
- Loss of consciousness – when a person loses consciousness, they may also lose control of their breathing or airway
- Respiratory failure – a condition where a person has difficulty breathing on their own
- Risk of aspiration – when a person is at risk of breathing in objects or substances that could block the airway
- Obstruction of the airway – when something is stuck in the respiratory tract, blocking the passage of air or oxygen
- Hypoxemia – a condition where an individual doesn’t have enough blood in their system, particularly in the arteries
- Neurological damage – refers to a wide range of conditions that mainly affect the nervous system
Failure to intubate successfully may result in death. Since videolaryngoscopy has better success rates, it is bound to replace direct laryngoscopy.
Awake Videolaryngoscopy Vs. Fibreoptic Intubation
Because of the advancement in technology that led to the development of awake videolaryngoscopy, FOI has been performed less frequently. While it’s not being ruled out completely as a procedure, awake videolaryngoscopy is quickly becoming the superior option for a variety of reasons.
Easier to Learn
Intubation expertise is easier to achieve with awake videolaryngoscopy than FOI. According to a Romanian Journal of Anaesthesia and Intensive Care article on awake videolaryngoscopy, an anesthetist can master intubation in one to six tries. For FOI, an anesthetist may need around 25 intubations to become an expert.
Effective Suctioning of Secretions
Videolaryngoscope creates space within the airway for effective secretion suctioning. It also permits suctioning of blood under direct vision. Plus, the space makes for better administration of atomized local anesthetic to the glottis and trachea when necessary.
No Blind Railroading or Diminution of View
Some of the FOI disadvantages are blind tube railroading and diminution of view when advancing towards the glottis. You encounter neither of these when performing awake videolaryngoscopy.
Though awake FOI used to be the most popular method, many anesthetists now avoid it because of its challenges. The technique is also much harder to learn. However, despite these factors, a review in the Singapore Medical Journal states that it’s still an essential skill to know.
Some patients may have difficult laryngoscopy or cervical spine injuries. In such cases, FOI would be the better option, however, it should only be the alternative or last resort.
Conclusion
For many medical experts, awake videolaryngoscopy is the superior option. Since science is always about improving, videolaryngoscopy is showing more advantages than traditional fiberoptic intubation among awake and anesthetized patients.
Both methods have similar success rates but video laryngoscopes are showing more successful and faster intubation times. Medical experts are always looking for better ways to successfully intubate during the first attempt since the procedure involves the airway, an essential part of breathing and surviving. Hence, awake videolaryngoscopy has proven to be a viable addition to intubation methods.
References
Chemsiam, RV. Bhananker, S. Ramaiah R. Videolaryngoscopy. Int J Crit Illn Inj Sci. 2014; 4(1): 35–41
Hodzovic, I. Bedread,O . Awake videolaryngoscope – guided intubation – well worth adding to your skill-mix. Anaesth Intensive Care. 2019 Apr; 26(1): 5–7
Wong, J. et al. Fibreoptic Intubation in Airway Management: A Review Article. Singapore Med J. 2019; 60(3): 110–118.
Moore, A. Schriker, T. Awake Videolaryngoscopy Versus Fiberoptic Bronchoscopy. National Library of Medicine. Curr Opin Anaesthesiol. 2019. ;32(6):764-768.
Davis, J. Bates, L. Rapid Sequence Induction Via an Intraosseous Needle. J Intensive Care Soc. 2016; 17(2): 178–179.
