However, once they finish their studies and training, many physicians rarely use emergency procedural techniques in clinical practice. Their exposure to such situations is limited, and their skills and knowledge may atrophy over time.
Here we delve into skill retention after emergency simulation-based training for various emergency procedures, such as lumbar puncture, paracentesis, thoracentesis, and central venous catheter (CVC) insertion.
What are emergency simulators?
Emergency simulators refer to educational tools and techniques used to train healthcare providers and professionals in various emergency procedures and critical skills. These simulators are designed to replicate real-life emergency scenarios, allowing practitioners to practice and hone their skills in a controlled, risk-free environment. They are commonly used to improve the knowledge and competency of healthcare professionals in responding to life-threatening situations. These skills encompass a wide range of emergency procedures, including but not limited to:
- Intubation: Inserting a tube into a patient’s airway to ensure proper breathing.
- Cricothyroidotomy: A surgical procedure to create an emergency airway.
- Pericardiocentesis: Draining fluid around the heart.
- Tube thoracostomy: Inserting a chest tube to relieve pressure in the chest cavity.
- Central line placement: Inserting a catheter into a major vein for various medical purposes.
Simulation based training involves creating scenarios that require healthcare professionals to apply these skills and make critical decisions, just as they would in a real emergency. These simulators can be physical mannequins or computer-based virtual simulations. The training helps medical practitioners refresh their knowledge and skills, ensuring they can respond effectively and safely when faced with critical situations.
Retention of Procedural Skills After Simulation Based Training
Physicians in other specializations very rarely need to employ critical emergency procedural skills in their daily work. Nonetheless, retaining these skills is essential, as they will be vital in responding to emergencies.
A 2020 systematic review analyzed studies wherein nonsurgical physicians performed these procedures using simulations:
- Intubation
- Cricothyroidotomy
- Pericardiocentesis
- Tube thoracostomy
- Central line placement
The studies under review looked at procedural skill performance right after and three months after simulation training. The review found that post-simulation course skill retention largely declined over time, although a few studies offered some proof of skill retention after simulation training.
Also, a 2012 systematic review on knowledge and skill retention of adult advanced life support in medical professionals found that skills decline considerably six to 12 months after completing courses. However, retaining basic procedural skills is easier than more advanced techniques.
Simulation training clearly has its limitations. Although procedural knowledge and skills increase after simulation exercises, the skill retention declines after 6-12 months.
That said, simulation is a great way to increase opportunities for training and exposure to emergency skills. They are excellent tools that help doctors, nurse pracitioners, ER physician assistants, and other healthcare professionals treat critically ill patients immediately and safely.
A 2015 review reported improved psychomotor performance skills with frequent neonatal resuscitation skills training. Ongoing simulation training helps doctors refresh their skills and knowledge and perform procedures more effectively in emergencies.
Regular assessments for skill retention may also help determine the best frequency of refresher education and boost skill development and overall retention in the long run.
A 2020 observational study showed that implementing a monthly trauma procedural and simulation training program enhanced the performance of surgical residents and the time for certain interventions.
However, more studies are needed to determine the optimal form of simulation training, whether it’s only testing skills as opposed to a full retraining session. Also, researchers need to study the appropriate time intervals in critical emergency skill re-exposure to maintain optimal skills and knowledge.
Simulation Training for Lumbar Puncture
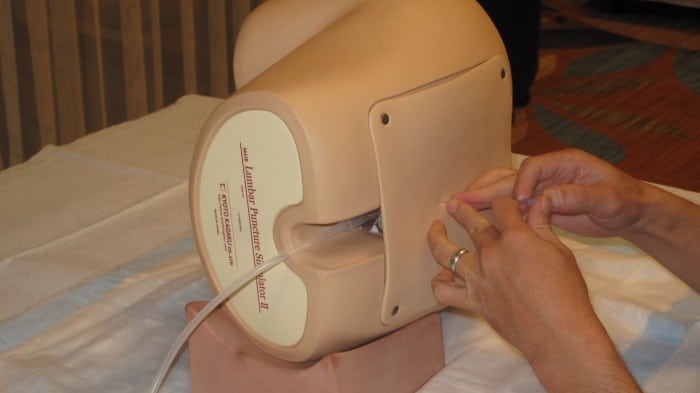
Lumbar puncture (LP) or spinal tap is a medical procedure that doctors perform across specialties. This invasive procedure involves some risks if not done correctly. But physicians can minimize risk with the proper knowledge and regular procedural practice.
A 2021 study showed that students’ know-how and confidence significantly improved after simulation training. It also led to a higher success rate of the first pass lumbar puncture in patients than those who did not receive simulation training. Students who went through simulation training also needed technical assistance less often.
Simulation based training is a fantastic tool that can help boost theoretical knowledge and practical skills and improve the safety and effectiveness of lumbar punctures.
Simulation Training for Abdominal Paracentesis
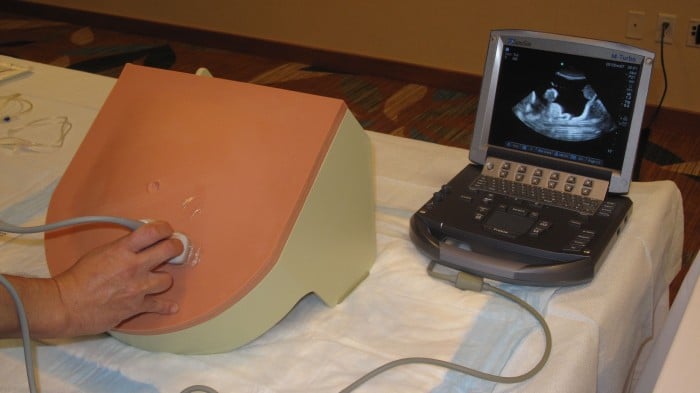
A 2019 study reported that simulation training for abdominal paracentesis helps students gain the requisite clinical skills in a safe learning environment before performing the procedure in real life. This method helps them avoid common risks and improve patient outcomes, so it is highly recommended for learning about the procedure.
Simulation Training for Thoracentesis

Clinicians can tackle the issue through simulation-based mastery learning (SBML). A 2018 randomized trial assessed the impact of SBML for thoracentesis on patient complications like hemothorax, iatrogenic pneumothorax (IP), and reexpansion pulmonary edema (REPE).
Resident doctors with SBML training who performed thoracenteses dealt with fewer clinically meaningful complications than those who received traditional training.
So, simulation training can significantly improve the effectiveness and safety of these procedures.
Simulation Training for CVC Insertion
A 2017 study demonstrated that central venous catheter (CVC) insertion skills can improve with standardized simulation training. Performing well during simulation-based testing may improve overall Central line placement outcomes among trainees.
This holds true even for experienced and competent medical professionals who have performed the procedure previously. So, regular simulation-based refresher training for healthcare providers—irrespective of their experience level—can help maintain proficiency.
Conclusion
Simulation-based training offers many benefits, and regular refreshers, along with the application of the acquired skills, can improve overall procedural competency. Emergency Simulation training helps improve the proficiency of healthcare providers regardless of experience level, thus improving patient outcomes and safety.
Hospital Procedures Consultants, along with the Postgraduate Institute for Medicine, have created an excellent course for healthcare professionals. The Hospitalist Procedures, Trauma Procedures, and Emergency Procedures Course helps medical staff improve their knowledge, skills, and competence so they can perform all types of procedures with ease.
It tackles various procedures using a hands-on training approach in a safe and low-pressure learning environment, making it great for professionals of all skill levels.
Enroll in the course today or contact Hospital Procedures Consultants to know more.
Resources
Legoux, C. Gerein, R. Boutis, K. Barrowman, N. Pling, A. Retention of Critical Procedural Skills After Simulation Training: A Systematic Review. AEM Educ Train. 2021; 5(3): e10536.
Yang, C. Yen, Z. McGowan, J. Carrie Chem, H Chiang, W. Mancini, M. Soar, J. Lai, M. Huei, M. A systematic review of retention of adult advanced life support knowledge and skills in healthcare providers. Resuscitation. 2012;83(9):1055-60. doi: 10.1016
Wener, A. Nikende, C. Keifenheim, K. Martin Bosse, H. Lund, F. Wagner, R. Celebi, N. Zipfel, S. Weyrich, P. “Best Practice” Skills Lab Training vs. a “see one, do one” Approach in Undergraduate Medical Education: An RCT on Students’ Long-Term Ability to Perform Procedural Clinical Skills. PLoS One. 2013; 8(9): e76354.
Perlman, J. Wyllie, J. Kattwinkel, J. Wyckoff, M. Aziz, K. Ginsburg, R. Part 7: Neonatal Resuscitation: 2015 International Consensus on Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Science With Treatment Recommendations. Circulation. . 2015 20;132
Park, C. Grant, J. Dumas, R. Dultz, L. Shoutz, T. Does simulation work? Monthly trauma simulation and procedural training are associated with decreased time to intervention. Trauma Acute Care Surg. 2020.;88(2):242-248
Tejos, R. Chahuán, J. Uslar, T. Inzunza, M. Villagrán, I. Simulated training program in abdominal paracentesis for undergraduate medical students. Gastroenterol Hepatol. 2019;42(4):239-247
Barsuk, J. Cohen, E. Williams, M. Scher, J. Jones, S. Feinglas, J. McGahie, W. Simulation-Based Mastery Learning for Thoracentesis Skills Improves Patient Outcomes: A Randomized Trial. Randomized Controlled Trial. 2018 ;93(5):729-735.
Alsaad, A. Moss, J. Silver, S. Johnson, M. Central Line Proficiency Test Outcomes after Simulation Training versus Traditional Training to Competence. Ann Am Thorac Soc.. 2017.;14(4):550-554
