Indications for a paracentesis
PARACENTESIS COURSE- cont'd info
Indications
Diagnostic Paracentesis
– Evaluate etiology of new- onset ascites
– Rule out spontaneous bacterial peritonitis
– Follow-up of therapy for spontaneous bacterial peritonitis
Therapeutic Paracentesis
– Respiratory compromise in patients with massive ascites
– Management of refractory, cirrhotic ascites
– Adjunctive management of hepatorenal syndrome
Contraindications for a paracentesis
Contraindications
Absolute contraindications
– Acute abdomen requiring exploratory surgery
– Infected abdominal wall at the entry site
– Uncooperative patient
– DIC or significant fibrinolysis
Relative contraindications
– Severe bowel distension or bowel obstruction
– Multiple prior abdominal surgeries
– Pregnancy
– INR > 5 (INR > 2.5 on warfarin)
– Coagulopathy with PTT 1.5x upper limit of normal
– Incidence of severe hemorrhage 0.2%(N= 4,500 paracenteses)
– Bleeding is reduced with ultrasound- guidance
– Thrombocytopenia (Platelets<25k)
– Use of DOAC or fondaparinux
Complications of a paracentesis
Paracentesis Complications
Major Complications
– Bowel or bladder perforation
– Hemoperitoneum (0.2%)
– Hypotension with large volume paracentesis
– Hepatorenal syndrome
Minor Complications
– Persistent ascitic fluid leak (1 % risk)
-Stitch vs ostomy bag vs dermabond 1 mL injected 1 cm deep
– Metastatic seeding of needle tract (rare)
– Soft tissue infection at puncture site
– Abdominal wall hematoma
Equipment for a paracentesis
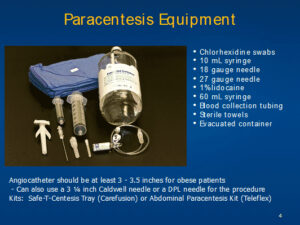
Paracentesis Equipment
- Chlorhexidine swabs
- 10 mL syringe
- 18 gauge needle
- 27 gauge needle
- 1% lidocaine
- 60 mL syringe
- Blood collection tubing
- Sterile towels
- Evacuated container
Angiocatheter should be at least 3 – 3.5 inches for obese patients
– Can also use a 3 ¼ inch Caldwell needle or a DPL needle for the procedure
Kits: Safe-T-Centesis Tray (Carefusion) or Abdominal Paracentesis Kit (Teleflex)
Proper positioning and technique for a paracentesis
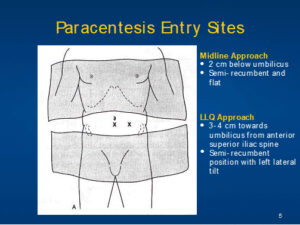
Paracentesis Entry Sites
Midline Approach
- 2 cm below umbilicus
- Semi- recumbent and flat
LLQ Approach
- 3-4 cm towards umbilicus from anterior superior iliac spine
- Semi-recumbent position with left lateral tilt
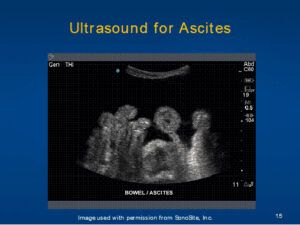
Ultrasound-directed paracentesis
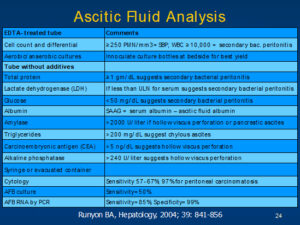
Ascitic fluid analysis
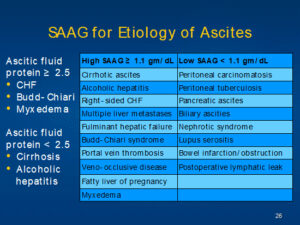
Serum- to- Ascites Albumin Gradient (SAAG)
SAAG ≥ 1.1 gm/ dL indicates that the patient has
portal hypertension (97% accuracy)
SAAG < 1.1 indicates that the patient has a cause of
ascites other than portal hypertension
Coding for a paracentesis
Coding for Paracentesis
- 49082 Abdominal paracentesis without image guidance
- 49083 Abdominal paracentesis with image guidance
– 52 Procedures that are incomplete or discontinued at physician’s discretion
– 53 Procedures that are discontinued because the patient’s life is endangered