
Immediate medical intervention is necessary to treat the possible infection, although clinical evaluation can be quite a conundrum. This is because there’s no way of knowing what caused the infection until the infant develops signs of the underlying disease or the lab work shows some indicative criteria.
How Do You Evaluate and Manage Infants With Fever?
The 1970s saw a rising concern for GBS infections among infants which led to extensive evaluations and treatments for all infants younger than 60 days. With the 1983 research, however, selective hospitalizations became a possibility.
In the 1980s and 1990s, experts from emergency departments started conducting research to determine methods that would make it easier to diagnose febrile illness.
But infants with fever is a broad area to research as it encompasses a variety of viruses or bacteria that could have compromised the health of the baby. That is why an attempt was made to separate urinary tract infections (UTI), which are quite common in infants, from invasive bacterial infection (IBI), which is prevalent in febrile neonates under 60 days of age and often includes bacteremia and meningitis.
During testing, the initial practice was to monitor peripheral white blood cell (WBC) count, band count, cerebrospinal fluid (CSF) analysis, and urine WBC count. Unfortunately, they had high negative predictive values, so there was no possible way to predict who was at risk and who wasn’t. Plus, the comprehensive testing was expensive.
Clinicians followed these guidelines in only 42% of cases while only 2 out of 3,066 infants had a missed invasive bacterial infection (IBI), although there were no adverse outcomes.
Due to the constantly evolving standards for testing, changing epidemiology of bacterial infections, increased immunization against Streptococcus pneumoniae, and improvements in food safety, the AAP (American Academy of Pediatrics) saw the need to establish a clinical practice guideline (CPG) for the management of infants with fever.
What Is the AAP’s New Practice Guideline?
Over approximately 10 years, they reviewed the literature available, then updated the guidelines according to advancements in the medical field. This helped them come up with protocols for three age groups: 8-21 days, 22-28 days, and 29-60 days.
The guidelines, which were released in August 2021, made it easier to determine which infants required extensive testing and which could be managed with outpatient services.
The guideline focused on the management of well-appearing febrile patients born at 37 weeks or later and those who exhibited temperatures of at least 100.4 degrees Fahrenheit in the previous 24 hours. It was also relevant for infants with upper respiratory tract symptoms, diarrhea (unless there is a high risk for bacterial pathogens), otitis media, etc.
What Are the Changes in AAP’s Updated Guideline?
According to the new guideline, infants 22 to 60 days old have a smaller chance of developing IBI during their first few months. Meanwhile, infants in their first week of life are excluded from the guideline as they could have different types of illness.
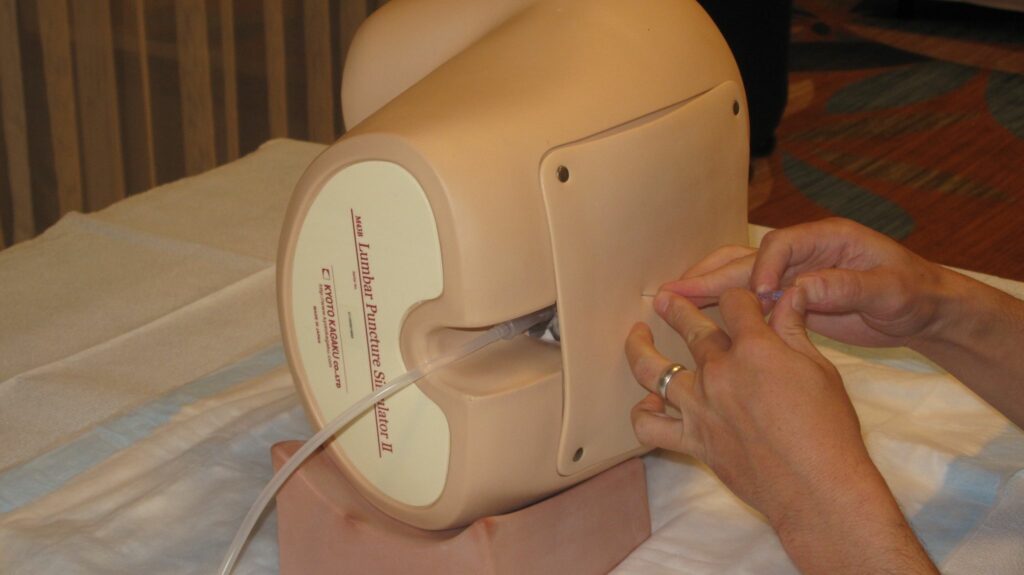
For infants aged 8 to 21 days, immediate hospitalization is a must. Their symptoms must be managed in the hospital and a lumbar puncture should be performed. They can only be discharged if their blood culture, CSF analysis, CSF culture, and UA (if it comes back positive, then urine culture) remained negative in the past 24 to 36 hours.
For infants who are 22 to 60 days old, their symptoms can be managed at home with verbal and/or written instructions from their doctors as long as their initial laboratory results and evaluation are normal. However, a follow-up within 24 hours is necessary to ensure the infant’s stable condition.
If the UA comes back positive, clinicians are to engage in shared decision-making to determine if a direct lumbar puncture among 22 to 28-day-old infants might be relevant. The procedure is meant to facilitate the early identification and treatment of meningitis. For babies aged one month and older, oral antibiotic therapy is the appropriate treatment method.
With the new guidelines, parents will have less anxiety and more peace of mind regarding their physicians’ care for sick infants. Doctors, on the other hand, can easily respond to an infant’s changing conditions by administering different treatments and giving intravenous antibiotics if necessary to ensure a speedy recovery.
The clinician has 21 key action statements (KASs) to adhere to. They must also communicate the risks and benefits of a particular testing or treatment with the child’s caregivers to ensure transparency. In addition, these discussions must be documented in the patient’s medical records.
Inflammatory Markers for Determining the Risk of IBI
Previously, the absolute neutrophil count (ANC), temperature, and WBC count were used to determine the risk of developing IBI. However, since they do not take into account the changing epidemiology of infections in infants, inflammatory markers, such as C-reactive protein (CRP), can be used as point-of-care testing.
While CRP is useful in the prediction of bacterial infections in infants with fever, procalcitonin levels may prove to be a better diagnostic solution than CRP for IBI.
If diagnosing a patient’s procalcitonin levels isn’t an option, CRP testing is still a viable alternative and provides results in under one hour.
Treatment Course
E-coli is the predominant Gram-negative organism and bacteria that causes neonatal bacteremia, surpassing group B Streptococcus (GBS) for neonatal meningitis in most studies.
If you follow protocols from the 1980s, there’s a significant risk of misclassification. Hence, the empirical antibiotic regimen that is decided with peers based on relevant perinatal history and laboratory results should take precedence.
Conclusion
While AAP’s guidelines provide more considerations and recommendations for infant care, factors like broad viral testing and the risk of concurrent IBI are still under research. Hence, the management of hospital procedures in febrile infants, particularly with sonographically-guided ultrasound, should be determined using various thresholds such as risk assessment and tolerance, differential access to care and reliability of follow up, Lumbar puncture is still an important consideration in the fever work-up of infants but physicians can use shared decision-making for patients aged 22-60 days old who appear well.
Resources:
Cole, B. Ilikj, M. McCloskey, C. Chavez-Bueno, S. Antibiotic resistance and molecular characterization of bacteremia Escherichia coli isolates from newborns in the United States. Research Article. 2019. July
McCulloh, R. McDaniel, Lauren. Kerns, E. Prevalence of Invasive Bacterial Infections in Well-Appearing, Febrile Infants. Hospital Pediatrics. 2021. September
DeAngelis, C. Joffe, A. Willis, W. Iatrogenic risks and financial costs of hospitalizing febrile infants. Am J Dis Child. 1983 Dec;137(12):1146-9
Pantell, R. Newman, T. Management and outcomes of care of fever in early infancy– JAMA 2004. Mar 10;291(10):1203-12
