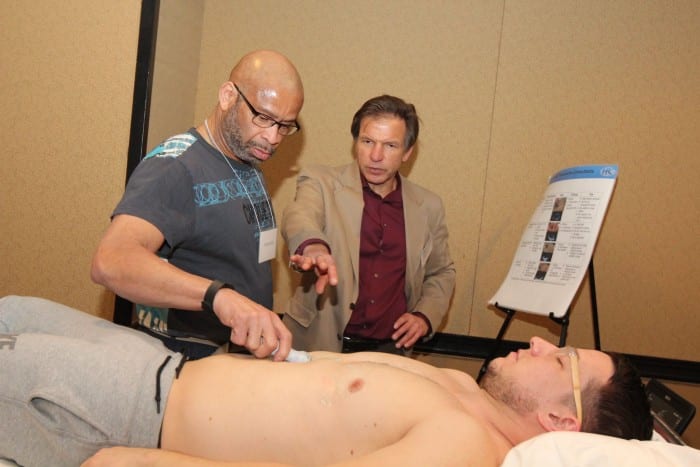
Around 80% of these traumatic injuries are blunt, with incidences of fatality secondary to hypovolemic shock and intraperitoneal bleeds. Fatalities can be prevented if professionals move fast with point-of-care ultrasound (POCUS).
With sonography, experienced diagnosticians can identify trauma quickly. The best-known application, valued for its high sensitivity and predictive value, is eFAST point-of-care ultrasound.
Learn how eFAST can help with Hospital Procedures Consultants:
What Is eFAST?
When it comes to traumatic injuries, learning what caused them can drastically improve patient outcomes.
Medical professionals once used FAST (Focused Assessment with Sonography in Trauma) as a diagnostic tool for POCUS in emergency departments. It focused on the presence of fluid in four areas: pelvic, pericardial, perihepatic, and perisplenic. However, it had significant limitations for detecting retroperitoneal fluid and bypassed lung ultrasound.
And so, in the mid-2000s, the evaluation of the thorax was added to FAST, leading to eFAST (Extended Focused Assessment with Sonography in Trauma).
eFAST ED can accurately identify pneumothorax and free fluid in the anterior and lateral pleural spaces in a trauma setting to ensure rapid evaluation of pneumothorax and/or hemothorax. It gives clinicians an accurate go-ahead for interventions (for example, tube thoracostomy or diagnostic laparotomy) or helps them with further diagnostic testing.
What Are the Indications of the eFAST Exam?
The introduction of the eFAST protocol in 2004 has changed the diagnostic landscape.
The eFAST exam brought ease of use to the fore for assessing free fluid in case of trauma while being non-invasive and without ionizing radiation. This means it does not have contraindications, even in pregnant women.
It can be used in many scenarios, such as:
- Evaluation of stable blunt trauma (whether abdominal or thoracic)
- For hemodynamically unstable trauma patients
- Part of RUSH — Rapid Ultrasound for Shock
- Unexplained hypotension
- Identifying a rupture in an ectopic pregnancy or a ruptured ovarian cyst
eFAST ED can also be used to evaluate penetrating trauma. Keep in mind that the air in the peritoneal or pleural spaces won’t allow ultrasound waves to penetrate deeper. The results may not be as accurate, which can hamper diagnostics.
Diagnostic Accuracy of eFAST in Trauma
The eFAST exam is an accurate tool that is of great assistance in various clinical situations. It has high sensitivity and specificity.
A review of the present literature looked at 75 studies between 1989 and 2017. It showed that the test has 69% sensitivity and 99% specificity for detecting pneumothorax. This eFAST exam has an 80% sensitivity and 75% specificity for detecting free fluid in abdomen and is why it has replaced diagnostic peritoneal lavage (DPL), an invasive test used to detect intraperitoneal hemorrhage or ruptured hollow viscus in trauma patients. eFAST can also provide precise results without needing an X-ray.
That said, it would be wise to note that the diagnostic accuracy of the E-FAST exam fluctuates based on injury. Here are two examples to illustrate this statement:
- In the case of pericardial effusion, the test has 91% sensitivity and 94% specificity.
- In the case of intra-abdominal free fluid, the test has 74% sensitivity and 98% specificity. This can be further divided into groups: hypotensive (74% sensitivity and 95% specificity) and pediatric patients (71% sensitivity and 95% specificity) in the detection of free fluid.
For best results, clinicians must first evaluate the right paracolic gutter, as fluid flows to the right and the area is less obstructed than the left.
The initial evaluation is often effective, so it can reduce the time of operative intervention. This impacts the patient’s length of stay and survival rate.
That is why the EAST (Eastern Association for the Surgery of Trauma), Western Trauma Association, and ATLS all recommend using eFAST in the care of traumatic injuries. This means an estimated 96% of level 1 trauma institutions have added the test to their point-of-care sonography algorithms.
Does eFAST ED Have Any Limitations?
As with every technological advancement, the good comes with the bad. The eFAST ED protocol is no exception.
It has several limitations, such as:
It could result in a false negative: This could occur when the amount of fluid is less than 100 to 200 mL or the minimum requirement for visualization. And while it may be safely repeated several times to check the patient’s status, this wouldn’t be of much help in an emergency or time-sensitive situation.
It could result in a false positive: This could happen in the setting of intravascular or intraperitoneal free fluid present before the traumatic injury. For example, a ruptured ovarian cyst, a recent peritoneal lavage, or peritoneal dialysis.
Here’s where it gets even trickier.
At times, free fluid in the abdomen may not even be a cause of concern; A full urinary bladder extending into the abdominal cavity can be mistaken as free fluid.
This is why it is extremely important to have skilled, experienced providers to interpret the ultrasound images from eFAST, which is crucial in the early resuscitation phase. The efficacy and accuracy of their diagnosis will influence decision-making if different providers perform follow-up scans.
In Conclusion
The eFAST ED exam is for finding the general region of bleeding, which could help clinicians determine the correct approach to minimize the fatality risk.
However, as eFAST exam results depend on the operator’s expertise, it would be a good idea to train in this technique with Hospital Procedures Consultants. This course tackles the latest techniques and best practices for proper probe positioning and how to interpret ultrasound images to quickly assess signs of free fluid. It will be easier to incorporate these findings into management decisions for effective intervention.
Enroll in the course today or contact Hospital Procedures Consultants to know more.
Resources
Brun, P. Bessereau, J. Chenaitia, H. Pradel, A. Denial C. Garbaye, G. Melaine, R, Bylicki, O. Leblanc, C. Stay and play eFAST or scoop and run eFAST? That is the question!. Randomized Controlled Trial. 2014. 32(2):166-70
Netherton, S. Milenkovic, V. Taylor, M. David, P. Diagnostic accuracy of eFAST in the trauma patient: a systematic review and meta-analysis. Meta-Analysis. 2019. 21(6):727-738
Richards, J. McGahan, J. Focused Assessment with Sonography in Trauma (FAST) in 2017: What Radiologists Can Learn. 2017
Bloom, B. Gibbons, R. Focused Assessment with Sonography for Trauma
Taghavi, S. Nassar, A. Askari, R. Hypovolemic Shock. Continuing Education Activity.
Whitehouse, H. Weigelt, J. Diagnostic peritoneal lavage: a review of indications, technique, and interpretation. Scand J Trauma Resusc Emerg Med. 2009. 8
Reza, M. Hadi, M. Ebrahimi, A. Samimi, K. Rezaee, M. Reza, H. Kazemi, H. Accuracy of Rapid Ultrasound in Shock (RUSH) Exam for Diagnosis of Shock in Critically Ill Patients. Trauma Mon. 2015 20(1)
Kumar, S. Kumar, V. Kumar, D. Sharma, P. Accuracy of Focused Assessment with Sonography for Trauma (FAST) in Blunt Trauma Abdomen—A Prospective Study. Indian J Surg. 2013. 393–397.
Savatmongkorngul, S. Wongwaisayawan,S. Kaewlai,R. Focused assessment with sonography for trauma: current perspectives. Open Access Emerg Med. 2017; 9: 57–62
Devadoss, H. Sharma, P. Nair, V. Rehsi, S. Roy, N. Rao, P. Diagnostic Accuracy of e-FAST in Stable Blunt Trauma Chest: A Prospective Analysis of 110 Cases at a Tertiary Care Center. Indian J Crit Care Med. 2021; 25(10): 1167–1172
Lucas, B. Hempel, D. Otto, R. Brenner, F. Stier, M. Prehospital FAST reduces time to admission and operative treatment: a prospective, randomized, multicenter trial. Eur J Trauma Emerg Surg. 2022; 48(4): 2701–2708
